Can a vasectomy reversal be successful after 10 years?



 December 05 / 2025
December 05 / 2025
So what is the recovery like after a vasectomy reversal? To some degree it depends on technique. We employ a single incision, mini-incision technique where the access point to perform the vasectomy reversal is about 1 cm. This is all designed to get patients back up on their feet and back to normal activities as quickly as possible.
We generally advise patients that it takes about 7 to 10 days to feel back to “normal” after a vasectomy reversal. Light activity, walking, office work, driving can essentially happen right away. We want to avoid heavy, strenuous physical activity for about 2 to 3 weeks.
After 2-3 weeks, patients can test things out. If things are still sore and sensitive, you just back off and take it a bit slower for another week. Give yourself a little bit more time. But generally speaking, 7 to 10 days is what it takes for our patients to feel back to normal after a vasectomy reversal. Hope this is helpful. Please email me directly with any questions:
 How painful is a vasectomy reversal? The truth is not too bad at all. In fact, many patients tell us that it is not as bad as the vasectomy itself, which is performed under local anesthetic, with the patient awake and aware of their circumstances so it can be a bit of an intimidating and anxiety provoking situation. Vasectomy reversals are performed typically with patients asleep, either with a general anesthetic or sedation, and they don't feel very pain much at all during the operation. After the procedure, their pain is controlled simply with Tylenol and an anti-inflammatory, and that really does the trick, and that's all that most patients need. We typically avoid narcotics altogether, as they are really not necessary. Patients typically say the most painful part is paying for the operation. Ouch. Sorry about that. Please email me directly with any questions:
How painful is a vasectomy reversal? The truth is not too bad at all. In fact, many patients tell us that it is not as bad as the vasectomy itself, which is performed under local anesthetic, with the patient awake and aware of their circumstances so it can be a bit of an intimidating and anxiety provoking situation. Vasectomy reversals are performed typically with patients asleep, either with a general anesthetic or sedation, and they don't feel very pain much at all during the operation. After the procedure, their pain is controlled simply with Tylenol and an anti-inflammatory, and that really does the trick, and that's all that most patients need. We typically avoid narcotics altogether, as they are really not necessary. Patients typically say the most painful part is paying for the operation. Ouch. Sorry about that. Please email me directly with any questions: 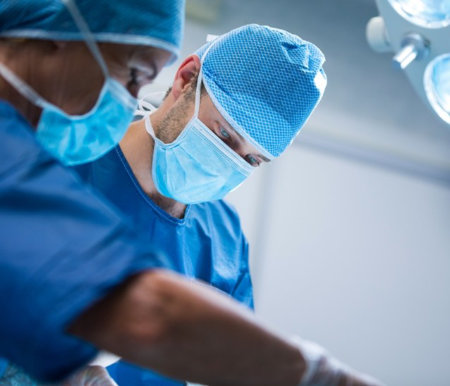

 Should you be getting your sperm count checked prior to vasectomy reversal to make sure that the vasectomy was successful and that no sperm are getting through? It's actually a reasonable question given that only 20 to 30% of men actually check to see that their vasectomy worked. The reality is however that vasectomies are 99.9% effective in terms of preventing babies. And if you did go for a sperm count, it's almost certainly to show no sperm at all, or extremely rare sperm getting through - which are not likely going to be helpful in terms of achieving a pregnancy. So, a sperm count prior to a reversal is not recommended as a necessary step. Please email me directly with any questions:
Should you be getting your sperm count checked prior to vasectomy reversal to make sure that the vasectomy was successful and that no sperm are getting through? It's actually a reasonable question given that only 20 to 30% of men actually check to see that their vasectomy worked. The reality is however that vasectomies are 99.9% effective in terms of preventing babies. And if you did go for a sperm count, it's almost certainly to show no sperm at all, or extremely rare sperm getting through - which are not likely going to be helpful in terms of achieving a pregnancy. So, a sperm count prior to a reversal is not recommended as a necessary step. Please email me directly with any questions:  December 06 / 2025
December 06 / 2025
Questions regarding the success of a vasectomy reversal are probably the most common and important questions I get. And not unlike the answers to most important questions, it depends…
Succes rates after a vasectomy reversal depend fundamentally on how you define success. Are we talking about sperm returning to the ejaculate? A pregnancy after a vasectomy reversal? Or the delivery of a healthy baby? They’re all quite different end points of success.
So let’s play this out.
Return of Sperm: One measure of success is sperm - more specifically the return of sperm to the ejaculate after a vasectomy reversal. After a vasectomy there should be no, none, zero sperm in the ejaculate. And so a “successful” vasectomy reversal could reasonably defined as the return of sperm to the ejaculate.
This is where you might see some specialist claiming a 99.9% success rate. Truthfully, I think that’s very misleading. Return of sperm to the ejaculate is VERY important. It’s the first critical step. But the devil is in the details. For example, a few dead or non-moving sperm in the ejaculate after a vasectomy reversal could technically be characterized by some as a “success” - sperm are technically present in the ejaculate – but that degree of sperm quantity and quality (a few dead or non-moving sperm) is very unlikely to result in a pregnancy or baby - which is ultimately what couples strive for.
The presence of good concentrations of live, actively moving sperm in the ejaculate is a much more meaningful indicator of success. Moreover, the amount or concentration of moving sperm really needs to be measured in a reliable way, at an experienced laboratory.
In our experience, about 90 to 95% of men will have live active sperm return to the ejaculate following a vasectomy reversal - but there’s a caveat to that which I’ll discuss in a bit.
Pregnancy after a vasectomy reversal: OK, now the presence of live active sperm in the ejaculate is great, but achieving a pregnancy and delivering a healthy baby is really the ultimate definition of success and the presence of sperm in and of itself does not = a baby. In our experience, about 2/3 of couples or about 60 to 75% are able to achieve a pregnancy following of vasectomy reversal.
Even with the availability of good quality sperm, baby making is influenced by a series of complex factor factors. For starters, another person factors into the equation - the female partner. And their age, overall and reproductive health and egg quality are really important determinants of successful baby making. Sperm and egg need to be compatible.
Relationship factors are also important. Some couples may try for a period of time and then may take a break or stop altogether. Some relationships unfortunately don’t last.
Other important determinants of success are the training and experience of the surgeon performing the vasectomy reversal. Not only is their surgical proficiency and skill important, but also their ability to exercise good judgement during the surgery to ensure the most appropriate and reliable vasectomy reversal connections are performed.
Technical factors are essential determinants of success with vasectomy reversal. How the reversal was performed makes a big difference. Was it microsurgical or performed using a surgical microscope (without question the gold standard) or performed without the use of magnification?
What type of reconnection were required and what type of reconnection was performed? They actually can be two different things. Direct vas to vas reconnections or a vasovasostomy (VV) are the most reliable types of connections and generally result in live active sperm returning to the ejaculate in 90 to 95% of cases. However, sometimes direct connections are not indicated and a bypass connection is necessary aka vasoepididymostomy (VE). If a bypass connection is required, we know that those connections are much more delicate and less reliable than direct connections and we typically see live active sperm return to the ejaculate in approximately 75% of patients. That’s the caveat I mentioned earlier.
It’s important to appreciate, that depending on the training and experience of your surgeon, not all doctors performing vasectomy reversals are comfortable completing a microsurgical bypass connection or VE, and will only perform a direct vas to vas reconnection or VV in all circumstances. Unfortunately, we know that if a bypass connection is indicated and not performed, it really compromises the success of the vasectomy reversal. All that to really say that choosing a surgeon with the right experience is really critical to success.
So back to the original question and to summarize things. What is the success rate of a vasectomy reversal?
Ideally couples should expect the return of live active sperm to the ejaculate in over 90% of cases. With that, approximately 60 to 75% of couples are able achieve a pregnancy following of a vasectomy reversal. Please email me directly with any questions:
 December 07 / 2025
December 07 / 2025
Hello everyone. This post comes to you from Montreal where I am with my son at a hockey tournament just drinking Tim Hortons. What could be more Canadian? I'm just answering a few emails between games and one thing that came up that I think is very relevant is - when can couples resume sexual activity after a vasectomy reversal? It's a really good question.
We really want to avoid a muscular contraction of the delicate tubes (vas) that were just brought back together during the vasectomy reversal surgery. The vas are tubes primarily composed of muscle tissue that contract with ejaculation (not just sex). That contraction may cause tension and disruptions of connections and possibly lead to separation, inflammation and pain.
I generally recommend avoiding ejaculation (not just sex) for about 2 to 3 weeks after surgery with resumption of sexual activity after that as long as guys are feeling perfectly normal. If still sore, wait another week.
This guideline tends to be a little bit more aggressive than some of my colleagues, but in my experience, I think there's nothing really wrong with that. So, hold off from sex (and ejaculation) for 2 to 3 weeks. That's the best I can do for you guys. Good luck! Please email me directly with any questions: